

Understanding Celiac Disease and the Relationship to Gluten Sensitivity
Retired
Celiac disease occurs for some people who have a problem processing gluten, which is a protein found in many foods. The gluten triggers an immune response that is not normal and damages the inside of the small intestine. Once that happens it is difficult to absorb the nutrients needed from the foods eaten.
What is Celiac Disease?
Celiac disease is the only known curable autoimmune disorder which occurs due to a genetic (inherited) susceptibility to the environmental trigger, gluten. Genetic risk is conveyed along the Human Leukocyte Antigen gene, HLA DQ2 (95%) and HLA DQ8 (5%). However, with the development of genome wide association studies (studies that look at the entire genetic code and attempt to link certain genes to specific diseases), it appears that there are 40 more candidate genes that may play a role in determining which of these HLA carriers will actually be the 4% of people who develop "full-blown" celiac disease. These 40 new genes convey only a very small contribution to the risk; however, the net effect of these genes likely contribute to at least 50% of the risk of developing celiac disease. In summary, whether someone develops celiac disease or not is very complicated!
Celiac Disease is Autoimmune
Celiac disease is autoimmune by definition and is, in fact, the only curable autoimmune disease with a known environmental trigger: gluten. Gluten is the primary structural protein complex of wheat with toxic fragments called gliadin and glutenin. Other grains, such as rye and barley, contain similar toxic elements as wheat gluten and therefore people can react to these other grains in a similar manner as wheat.
There are other types of immune reactions to wheat gluten, but we will focus on autoimmunity and celiac disease in this discussion.
In celiac disease, gluten causes activation of T-cells within the gastrointestinal tract. The adaptive (humoral) immune system responds through the development of antibodies against gliadin and a host tissue enzyme call tissue-transglutaminase and the endomyseum. These antibodies lead to inflammation and damage to intestinal structures of the small bowel.
Transglutaminase is an enzyme family responsible for creating highly stable protein bonds. These bonds allow the organism to develop strong protective structures like skin, hair, and nails. Transglutaminase activity can be excessive and is thought to play a role in the accumulation of pathological protein deposits in neurodegenerative diseases like Alzheimer's. The endomyseum is the connective tissue matrix surrounding muscle and contains transglutaminase.
Diagnosis of Celiac Disease
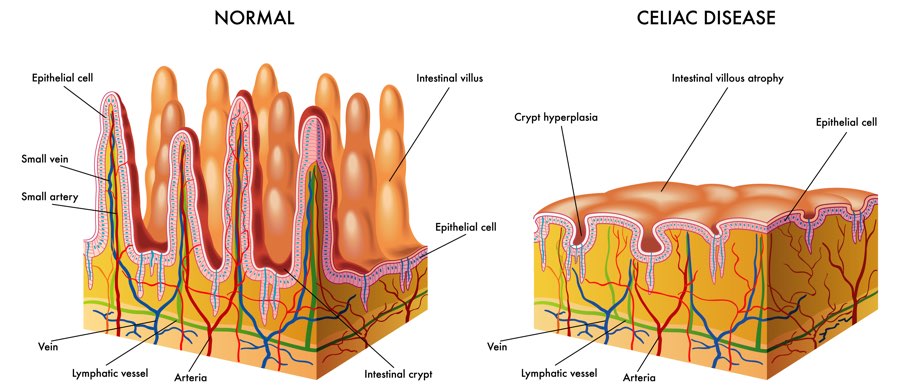
The diagnosis of Celiac Disease requires the presence of these autoimmune antibodies. It does not, however, require the finding of villous atrophy on endoscopic biopsy of the small intestine. The villi of the small intestine are microscopic finger like projects within the lumen of the small bowel that serve to increase the surface area exposed to the bowel contents. There are a variety of enzymatic, digestive and absorptive processes that occur "along" the villi. Chronic inflammation, triggered by gluten and perpetuated by anti-tissue transglutaminase, break down the villi. This diminishes the total surface area of the small intestinal mucosa as well as hampers the physiologic function of the cells that line the villi. The net effect of this process is villous atrophy, chronic immune activation, malabsorption, malnutrition, and increased risk for inflammatory bowel disease and cancer.
How is Gluten Sensitivity Different from Celiac Disease?
Gluten sensitivity (GS) is a well established response to gluten that is distinct from celiac disease. Whereas celiac disease is an autoimmune disease with an environmental trigger (gluten), gluten sensitivity is a symptomatic reaction to gluten that does not involve the autoimmune process. The presence of IgG and IgA to gliadin indicates that the patient has been exposed to gluten. The absence of antibody to self-tissues allows us to determine that celiac disease is not occurring.
Gluten sensitivity has symptom overlap to celiac disease, but does not involve tissue destruction (autoimmune disease). Small bowel villous atrophy, the classic diagnostic feature of celiac disease, is not present nor are there autoantibodies to human tissue. Digestive symptoms can be prominent in both entities. One unique aspect of GS from celiac disease is that gluten sensitivity activates the innate immune response, also called the cellular immune response (this is measured by a blood test called ALCAT). Furthermore, intestinal mucosal integrity is NOT compromised with gluten sensitivity, whereas celiac disease causes intestinal hyper-permeability (also called leaky gut).
Other unique feature with a non-celiac gluten reaction are its association with the neurological systems such as acute mania, schizophrenia, psychosis, multi-episode schizophrenia, and possibly autism. Many studies link gluten sensitivity to idiopathic neuropathy and what is now called gluten ataxia, whereby exposure to gluten appears to effect the cerebellar system (the balance center of your brain). From a genetic standpoint, only 50% of gluten sensitivity patients have the presence of HLA DQ2 or HLA DQ8, whereas these genetic markers are present in 100% of celiac disease patients.
SupplementRelief provides NuMedica's complete line of supplements for Gluten Sensitivity.


